Table of Contents
Overview
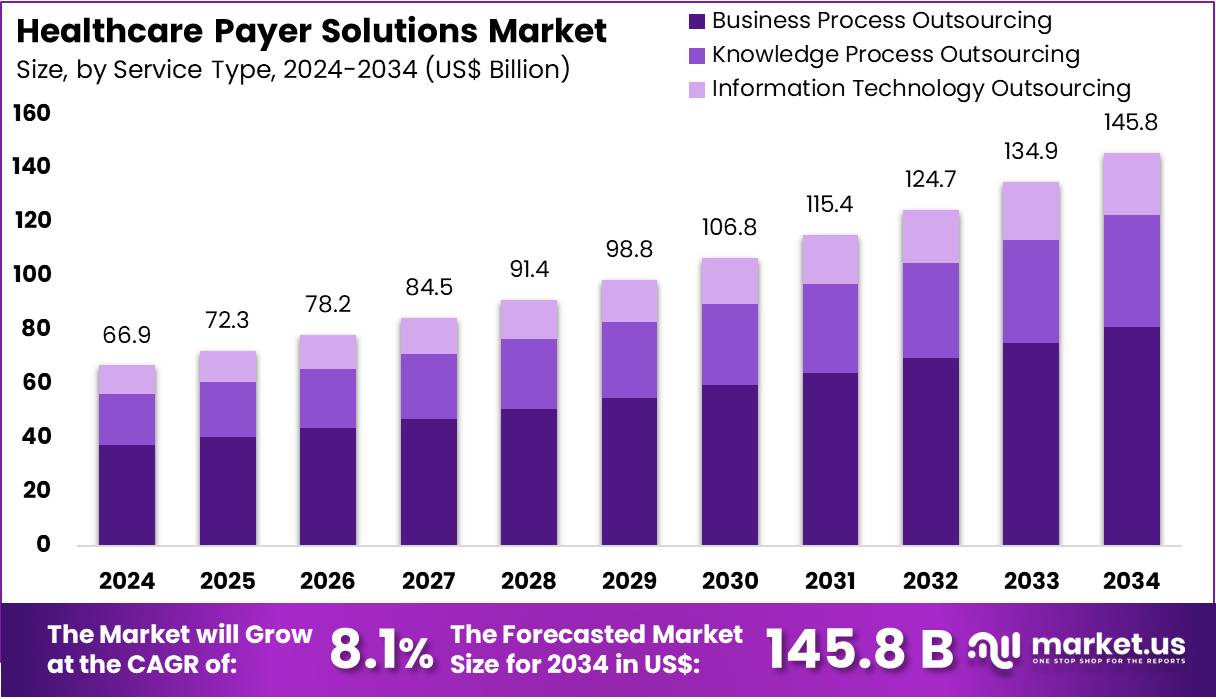
New York, NY – April 23, 2026 – The Healthcare Payer Solutions Market Size is expected to be worth around US$ 145.8 Billion by 2034 from US$ 66.9 Billion in 2024, growing at a CAGR of 8.1% during the forecast period 2025 to 2034.
Healthcare payer solutions refer to integrated technologies and services designed to support insurance providers, government health programs, and managed care organizations in optimizing operational efficiency and improving patient outcomes. These solutions typically encompass claims management, member enrollment, billing and payment processing, provider network management, and data analytics.
The increasing complexity of healthcare systems, combined with rising patient volumes and regulatory requirements, has driven the adoption of advanced payer solutions. It has been observed that digital transformation, including the integration of artificial intelligence, cloud computing, and automation, is enhancing the accuracy and speed of claims adjudication while reducing administrative costs.
Data analytics capabilities within payer solutions enable organizations to identify fraud, manage risk, and improve decision-making processes. Additionally, member engagement tools, such as digital portals and mobile applications, are facilitating better communication and personalized healthcare experiences.
Growth in the healthcare payer solutions market is being supported by the global shift toward value-based care models, where reimbursement is linked to patient outcomes rather than service volume. Interoperability and compliance with healthcare regulations remain key focus areas, ensuring secure data exchange and adherence to standards.
Overall, healthcare payer solutions are playing a critical role in transforming the healthcare ecosystem by improving efficiency, reducing costs, and enhancing the quality of care delivery across diverse healthcare settings.
Key Takeaways
- In 2024, the healthcare payer solutions market generated revenue of US$ 66.9 billion and is projected to reach US$ 145.8 billion by 2033, expanding at a CAGR of 8.1% over the forecast period.
- Based on service type, the market is categorized into business process outsourcing (BPO), knowledge process outsourcing (KPO), and information technology outsourcing (ITO). Among these, the BPO segment dominated the market in 2024, accounting for a leading share of 55.7%.
- By application, the market is segmented into claims management services, member management services, integrated front-office and back-office operations, provider management services, billing and accounts management services, analytics and fraud management services, payment management services, HR services, and audit and analysis systems. Claims management services emerged as the leading segment, capturing a market share of 24.6%.
- With respect to end users, the market is divided into private payers and public payers. The private payers segment held the dominant position, contributing the highest revenue share of 63.4% in 2024.
- Regionally, North America accounted for the largest share of the healthcare payer solutions market, representing 38.9% of the total revenue in 2024.
Regional Analysis
North America led the healthcare payer solutions market in 2024, accounting for a revenue share of 38.9%. This leadership is primarily driven by the growing need to manage escalating healthcare expenditures efficiently. In the United States, national health spending increased by 7.5% in 2023, reaching US$ 4.9 trillion, as per a December 2024 CMS report.
Such rising costs have accelerated the adoption of advanced payer solutions to enhance claims processing, cost control, and financial management. Additionally, the shift toward value-based care models, supported by CMS initiatives targeting full Medicare participation in accountable care arrangements by 2030, is further strengthening demand for advanced analytics and payment systems.
Asia Pacific is projected to register the fastest CAGR during the forecast period. Growth is being driven by expanding health insurance coverage through government initiatives and the implementation of universal healthcare programs. Increasing digitalization of healthcare infrastructure and rising concerns regarding fraud, waste, and abuse are further supporting the adoption of advanced payer solutions across the region.
Emerging Trends
- Adoption of artificial intelligence and automation is increasing across payer operations, enabling faster claims processing, improved fraud detection, and reduced administrative costs while enhancing overall operational efficiency and decision-making capabilities.
- Transition toward value-based care models is accelerating, where payments are linked to patient outcomes, encouraging payers to invest in care coordination, analytics tools, and outcome measurement systems for better healthcare delivery.
- Cloud-based platforms are being widely implemented, allowing scalable infrastructure, real-time data access, and seamless integration across systems, which supports cost reduction and improves flexibility in managing large volumes of healthcare data.
- Advanced data analytics and interoperability solutions are gaining importance, helping payers to generate actionable insights, predict health risks, and enable personalized healthcare strategies while improving collaboration between providers and insurers.
Key Use Cases
- Claims management solutions are utilized to automate claim submissions, adjudication, and reimbursements, reducing manual errors, accelerating processing times, and improving transparency across the healthcare payment lifecycle.
- Fraud detection systems are implemented to analyze large datasets and identify unusual patterns in claims, helping payers minimize financial losses, strengthen compliance, and maintain trust within the healthcare ecosystem.
- Member engagement platforms are used to provide digital access through portals and mobile applications, enabling better communication, improved customer experience, and higher retention through personalized healthcare services and information access.
- Care management solutions support population health initiatives by identifying high-risk patients, enabling preventive care strategies, and improving treatment outcomes while optimizing costs through efficient resource allocation and monitoring.
Frequently Asked Questions on Healthcare Payer Solutions
- What is the Healthcare Payer Solutions Market?
The healthcare payer solutions market comprises software, services, and platforms utilized by insurance payers to streamline operations, manage risk, and enhance customer engagement. Market growth is driven by digital transformation, regulatory requirements, and increasing demand for cost-effective healthcare administration systems. - What are the key components of Healthcare Payer Solutions?
Key components include claims management systems, provider network management, member engagement platforms, payment integrity solutions, and analytics tools. These components collectively enable efficient data processing, fraud detection, and improved decision-making capabilities within healthcare payer organizations. - What factors are driving the growth of the Healthcare Payer Solutions Market?
Market growth is primarily driven by rising healthcare costs, increasing insurance coverage, regulatory compliance requirements, and adoption of advanced technologies such as artificial intelligence and cloud computing, which enhance operational efficiency and improve service delivery across payer organizations. - How does digital transformation impact Healthcare Payer Solutions?
Digital transformation significantly enhances payer solutions by enabling automation, real-time data analytics, and improved customer engagement. Technologies such as AI, machine learning, and cloud platforms streamline operations, reduce errors, and facilitate personalized healthcare services for members. - Who are the primary users of Healthcare Payer Solutions?
Primary users include health insurance companies, government healthcare agencies, third-party administrators, and managed care organizations. These stakeholders rely on payer solutions to manage claims, control costs, ensure compliance, and improve operational transparency and efficiency. - What role does data analytics play in Healthcare Payer Solutions?
Data analytics plays a critical role by enabling predictive modeling, fraud detection, cost optimization, and improved patient outcomes. Advanced analytics tools help payers make data-driven decisions, enhance risk management strategies, and improve overall operational performance. - What are the emerging trends in the Healthcare Payer Solutions Market?
Emerging trends include increased adoption of cloud-based platforms, integration of artificial intelligence, focus on value-based care models, and expansion of telehealth services. These trends are reshaping payer operations and driving innovation across the healthcare ecosystem. - What is the future outlook for the Healthcare Payer Solutions Market?
The market outlook remains positive, with steady growth expected due to increasing healthcare digitization, regulatory demands, and demand for cost optimization. Continuous technological advancements and strategic partnerships are anticipated to further accelerate market expansion globally.
Conclusion
The healthcare payer solutions market is demonstrating steady expansion, supported by increasing healthcare complexity, rising costs, and ongoing digital transformation. Advanced technologies such as artificial intelligence, cloud computing, and data analytics are improving operational efficiency, claims accuracy, and decision-making processes.
The shift toward value-based care is further strengthening demand for integrated and outcome-focused solutions. North America remains a dominant region, while Asia Pacific is emerging as a high-growth market due to expanding insurance coverage and digital adoption. Overall, payer solutions are expected to play a critical role in enhancing cost efficiency, regulatory compliance, and quality of care delivery globally.
Discuss your needs with our analyst
Please share your requirements with more details so our analyst can check if they can solve your problem(s)



